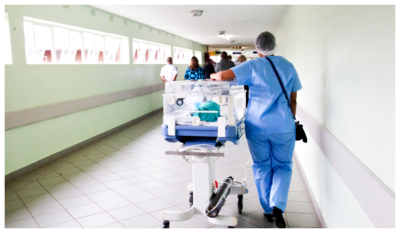
“Someone above needs to open up this conversation. Whether that be the health Secretary, or a key figure from the NHS…our voices matter.”
We’re living through very troubled and dangerous times right now, with more than four million around the world who have tested positive with Covid-19, and nearly 300,000 people who have died.
Now more than ever I am sparing my thoughts to those who are putting their lives on the line to treat people.
With the world recently celebrating International Nurses Day, I caught up with one nurse, who for the past month plus has been working at Nightingale hospital in London, which was built in nine days during the pandemic to treat Covid-19 patients.
The 28-year-old nurse Dorcas Boamah shares her experiences with me.
“No one expected or wanted this to happen. I remember in January when the previous hospital I was working in was prepping us for this pandemic, how to face it, and how to challenge it.
“In regards to social distancing and when this idea of movement was first introduced, it wasn’t really clear to begin with.
“We were just living our normal lives working. Then it suddenly became very serious.
“Death tolls were rising and rising, and then it came more clear to me that many of the patients I would see every day looked just like me.”

Recent reports have revealed the growing number of health workers in the NHS, who are more likely to die from Covid-19.
Public Health England were recently asked to start tracking coronavirus cases and deaths by ethnicity as part of the government’s review into why people from ethnic minority backgrounds were being disproportionately affected.
It comes after the majority of NHS healthcare workers who have died were from these backgrounds.
“Things were changing rapidly and I had to ask and prepare myself for what I was getting myself in for.
“I wanted to be in an unfamiliar environment with an unprecedented issue going on, that would give me an opportunity to improve the most in my job as a nurse.
“My mum and I prayed about it, and I felt an amazing peace in knowing this was the right thing to do..”
So in the nine years of working for the NHS, are these the worst possible conditions Dorcas has had to work in?

“Yes. It’s the most difficult thing I’ve ever had to do.” She says. “Physically, emotionally and mentally.”
“I usually start my day at 6:30am, get ready, and then walk to the Excel centre where the Nightingale hospital is based.
“My scrubs are usually on before I enter, then I will check in to be debriefed by my colleagues about what’s going on that day.
“We then get into our personal protective equipment also known as PPE, and are informed about how many patients we are expected to have, and what condition they’re in.
“When I’m on the wards so much happens; we have to keep an eye on the patient’s medication as many of them in critical condition need double pumping of medication, meaning that before one pump of medication runs out, another one needs to be running already.
“This happens commonly with patients who are sedated. And then there’s doing blood gasses every two hours for other patients in different conditions.
“My current hospital does a really great job at ensuring that the staff are checking in with our mental wellbeing.
“I check in on myself a lot, and my colleagues and I always look out for each other. We are seeing sick and dead people every single day, so mental check ins are so important.”
But how many more mental check-ins would a nurse from a black and minority ethnic background have to take, after realising that day by day, more victims from the same background are more likely to die from the same disease?
“On one of my earliest shifts, I remember walking into a unit and when looking down the corridor, almost every patient in sight was from an ethnic minority.
“This still has a massive effect on me. I cried so hard after. I thought ‘this could be my family.’ It makes it real. I saw it reported a lot in the media, but nothing can compare to seeing it in real life. This really brought it back home.
“Those on top need to address this issue more.
“From the types of management that I have seen from the Nightingale, I’ve seen a lot of them engaging with every single person and it’s not been like different types of hospitals that I’ve been in where the structure of management can be biased.
“Leadership need to engage with the people affected the most…it’s okay for a manager who is a white Caucasian to come to me and say, ‘Dorcas, you know, as we can both see, a lot of the people in this ward are from an ethnic minority…how are you feeling about this?’
“These conversations need to happen more internally.”
So what can be done?
“Someone above needs to open up this conversation. Whether that be the health Secretary, or a key figure from the NHS.
“But to be honest, I feel like anyone can play part of this. I’m seeing this movement shift especially by the many conversations being raised on social media.
“Our voices matter, and I’m grateful others are also speaking up for us.”
Written By: Hannah Ajala – freelance journalist – @hannah_ajala
Images Copyright – Interviewee own supplied images and edited by I Am New Generation Magazine / Shutterstock
More Stories
The young people, around the world, helping to fight Covid-19